Treatment Options
The aim of treatment is to reduce the impact of severe spasticity, to prevent further complications, and improve quality of life.1,2 This involves a team approach with coordinated management and communications between doctors, physician’s assistants, nurses, physical/occupational therapists, neurologists, physical medicine and rehabilitation specialists, orthopedists, and patients and their caregiver(s).1,3 Successful treatment means that the care plan has realistic and meaningful goals for each patient to meet their individual care needs for both functional improvement and quality of life.1,4
Treatments for severe spasticity can include:2,5
- Physical therapy/Occupational therapy
- Bracing/Splinting
- Oral medications
- Injectable medications
- Intrathecal baclofen therapy (ITB therapy)
- Surgery
Treatment Options for Severe Spasticity2,5
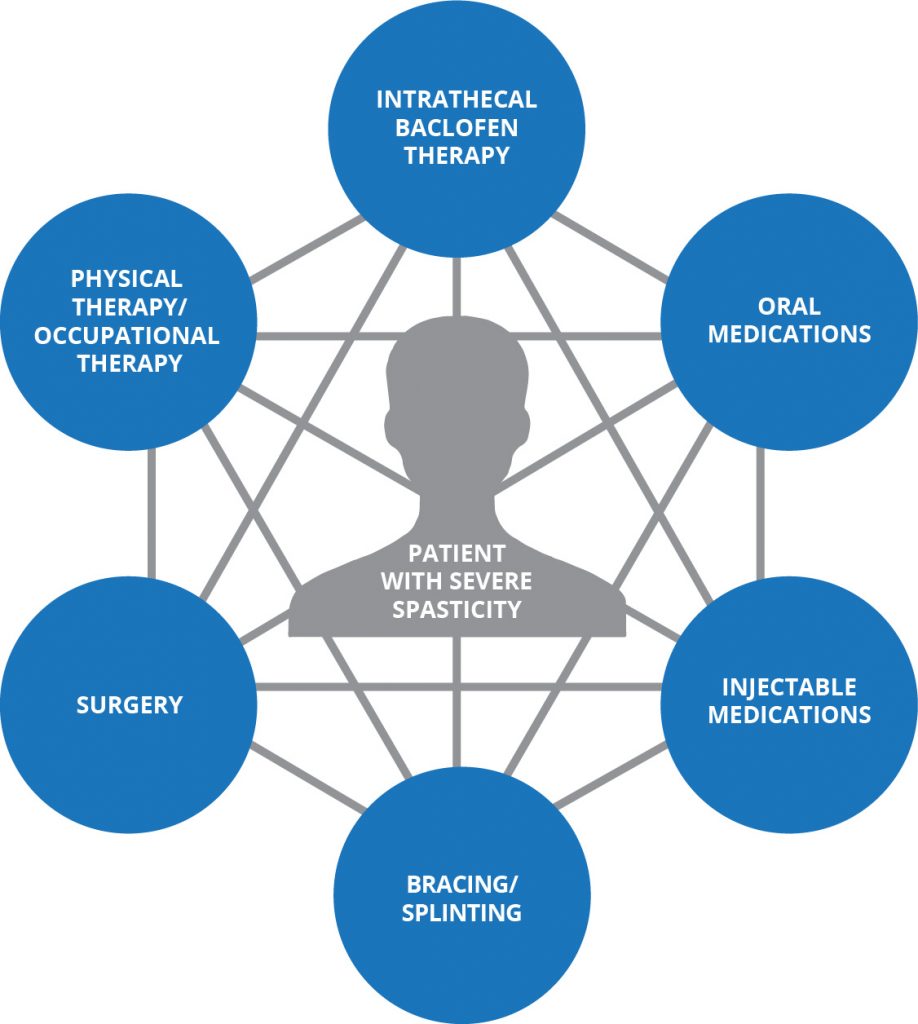

Each of these methods of treating spasticity has its own respective risks and benefits. For example, injections with botulinum toxin can be helpful in treating localized spasticity.2 Oral medications are easy to prescribe, but many people may experience adverse effects, such as sedation or inconsistent tonal reduction.2 ITB Therapy℠ with Lioresal® Intrathecal (baclofen injection) is an option for the management of severe spasticity that interferes with comfort, active or passive function, activities of daily living, mobility, positioning, or caregiver assistance.2 When current management of spasticity is inadequate or has caused intolerable side effects, ITB can be a preferred treatment option after spasticity has been evaluated for the degree of body involvement, progressive versus static disease, and particularly when spasticity is the result of cerebral or spinal origin.2
The most frequent drug adverse events with Lioresal® Intrathecal (baclofen injection) vary by indication, but include hypotonia (34.7%), somnolence (20.9%), headache (10.7%), convulsion (10.0%), dizziness (8.0%), urinary retention (8.0%), nausea (7.3%), and paresthesia (6.7%). Dosing or programming errors may result in clinically significant overdose or withdrawal.6
When to Consider ITB Therapy℠ with Lioresal® Intrathecal (baclofen injection)
Labeling for Lioresal® Intrathecal requires failure of oral medication prior to initiating ITB Therapy in spasticity of spinal origin.2 There is no precise definition regarding the duration of oral medication trial required, and an expert consensus panel strongly recommended proceeding quickly to ITB therapy in appropriately selected patients.2 Patients with spasticity due to traumatic brain injury should wait at least 1 year after injury before considering long-term ITB Therapy℠ with Lioresal® Intrathecal.6
Prior to implantation of a device for chronic intrathecal infusion of Lioresal® Intrathecal, patients must show a response to Lioresal® Intrathecal in a screening trial. Please review the dosing and administration section of the Lioresal® Intrathecal prescribing information for further details.
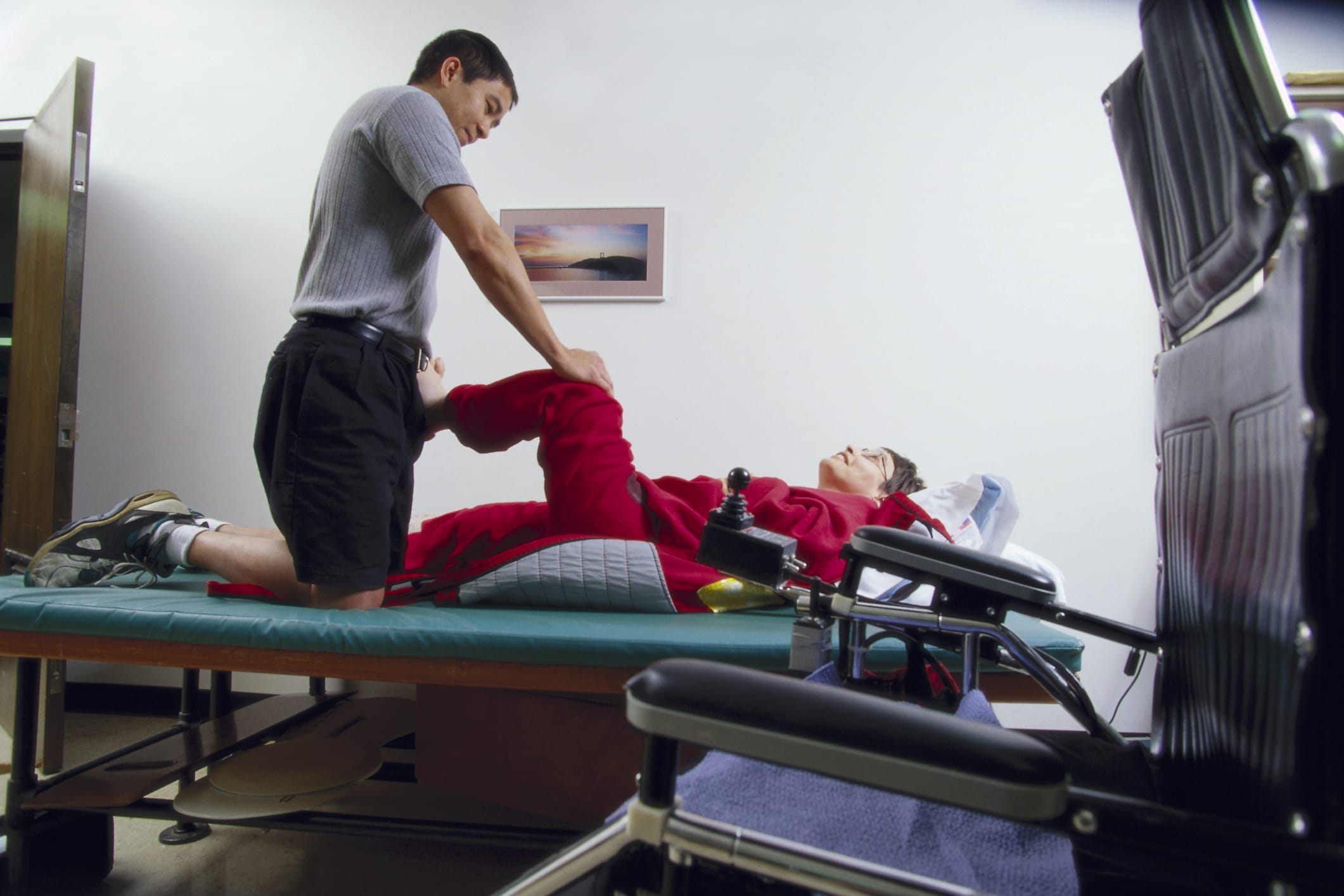
Other possible therapies include bracing, casting, surgery, and occupational or physical therapy.2 These options fail to eliminate the underlying muscle overactivity, but do provide supportive care and may be used in combination with medication to provide optimal outcomes for patients with severe spasticity.2
If other medications provide inadequate control of severe spasticity, undesirable or intolerable side effects, or fail to adequately meet quality of life goals, then consider ITB Therapy℠ with Lioresal® Intrathecal (baclofen injection).
- Nair KP, Marsden J. The management of spasticity in adults. BMJ. 2014;349:g4737.
- Saulino M, Ivanhoe CB, McGuire JR, et al. Best practices for intrathecal baclofen therapy: patient selection. Neuromodulation. 2016;19(6):607-615.
- Brashear A, Elovic E. Chapter 1: Why is spasticity treatment important? In: Brashear A., Ed. Spasticity. Diagnosis and Management. 2nd ed. Demos Medical Publishing, LLC. 2016.
- Elovic E, Brashear A. Chapter 9: Setting realistic and meaningful goals for treatment. In: Brashear A, Elovic E, eds. Spasticity: Diagnosis and Management. 2nd ed. New York, NY: Demos Medical Publishing, LLC, 2016.
- Spasticity. American Stroke Association (ASA) website. https://www.strokeassociation.org/STROKEORG/LifeAfterStroke/RegainingIndependence/PhysicalChallenges/Spasticity_UCM_309770_Article.jsp#.WEcdiXeZMp8. Updated November 22, 2016. Accessed December 7, 2016.
- Lioresal® Intrathecal (baclofen injection) for intrathecal injection [prescribing information]. Saol Therapeutics, Roswell, Georgia; January 2019.